Why Voice Is the Natural Interface for Clinical Documentation
Physicians are trained communicators. They ask precise questions, listen carefully, and synthesize complex information into clear clinical summaries. What they are not trained to do is type quickly while also paying attention to a patient. Yet that is exactly what electronic documentation requires. The disconnect between how physicians think and communicate naturally, through speech, and how documentation systems are built, requiring typed input, is a significant source of friction in clinical practice. Voice to medical notes technology addresses this mismatch directly.
How the Technology Works in Practice
Modern voice-to-notes systems go well beyond basic transcription. They do not simply convert speech to text and hand the output to the physician. Instead, they process spoken clinical conversations through AI models trained on healthcare language and documentation standards. The system identifies clinically relevant information, discards conversational filler, and organizes the content into structured note formats.
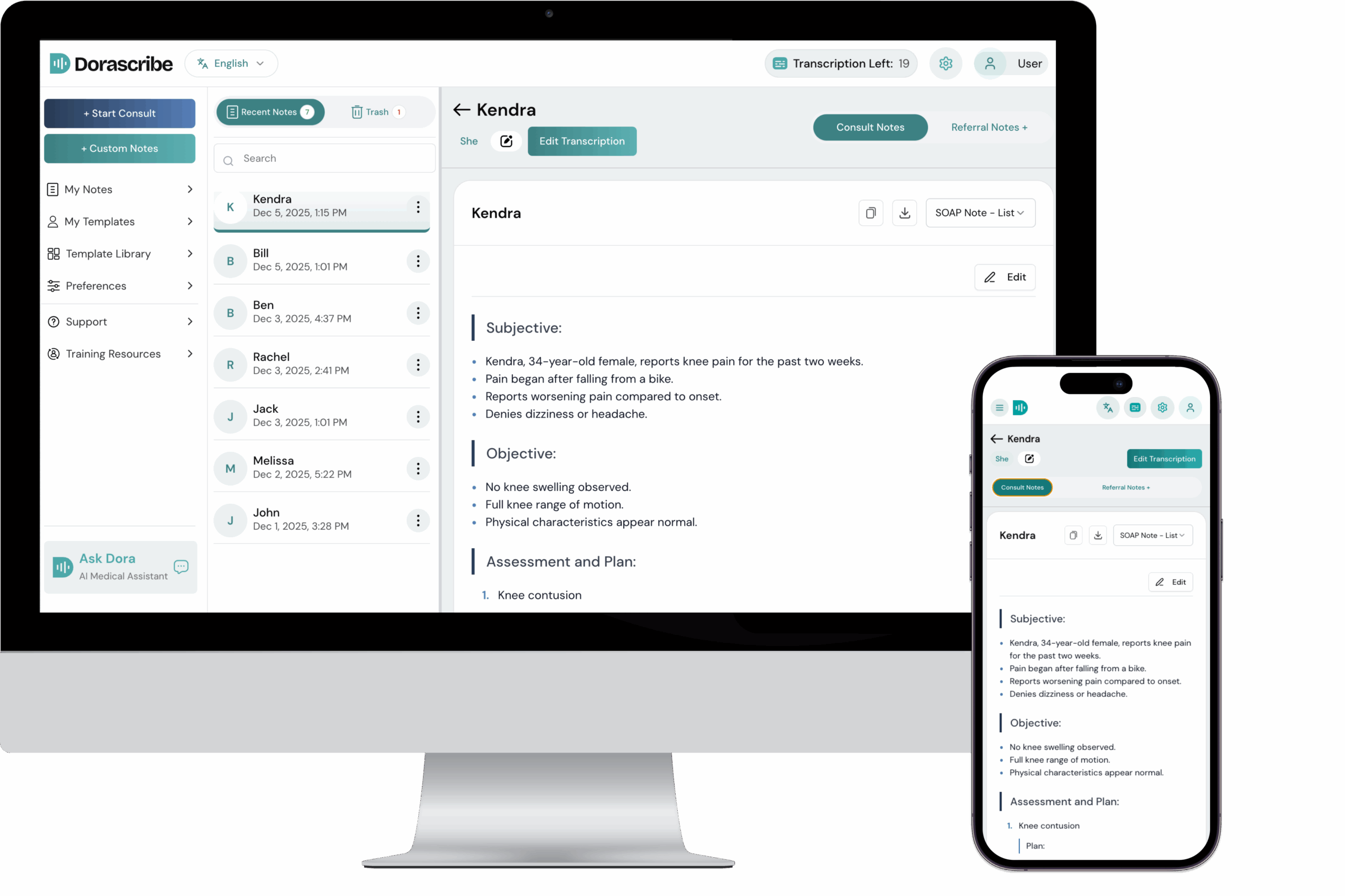
Platforms offering voice to medical notes functionality allow physicians to speak naturally during or after a patient visit, and the system handles the formatting, the template population, and the EHR entry. The physician reviews the output, makes any necessary corrections, and signs off. The whole process takes a fraction of the time that manual documentation requires.
Specialty-Specific Applications Worth Knowing
Voice-to-notes technology is particularly valuable in high-volume specialties where documentation demands are intense. Primary care, emergency medicine, and urgent care practices see some of the strongest ROI because of sheer encounter volume. But the technology is also gaining traction in hospital medicine, where physicians manage large inpatient panels and need to document rounds, assessments, and care plans across many patients each day.
Surgical specialties are another growing area of adoption. Operative reports, procedure notes, and post-operative assessments have traditionally been time-consuming documents to produce. Voice capture during or immediately after procedures makes this much more manageable.
Addressing Common Concerns About Accuracy
The most common hesitation physicians express about voice-to-notes systems is accuracy. Clinical documentation errors can have genuine patient safety implications, and understandably, physicians want to be confident before relying on any AI-generated note.
Current leading platforms achieve accuracy rates that compare favorably with human scribes, and they continue improving as they process more clinical data. The review step in the workflow serves as an important safety layer, ensuring the physician confirms the note before it becomes part of the permanent record. Most experienced users report that their review process becomes faster and more efficient as they grow familiar with the platform.
Conclusion
The shift toward voice to medical notes is gaining momentum for good reason. It aligns documentation technology with the natural way physicians communicate, reduces administrative burden, and ultimately allows more attention to flow where it belongs, toward the patient in the room.

